Dentistry is our profession
With the art of healing and sciece we are devoted to maintain your oral health.

Invisalign Treatment
Looking to straighten your teeth without the use of metal braces? Invisalign is comfortable and easy to use orthodontic treatment that uses a serie...

Dental Emergency
Dental emergencies are often painful and inconvenient, but with the right care youll feel better in no time. Overall, toothaches, teeth that ar...
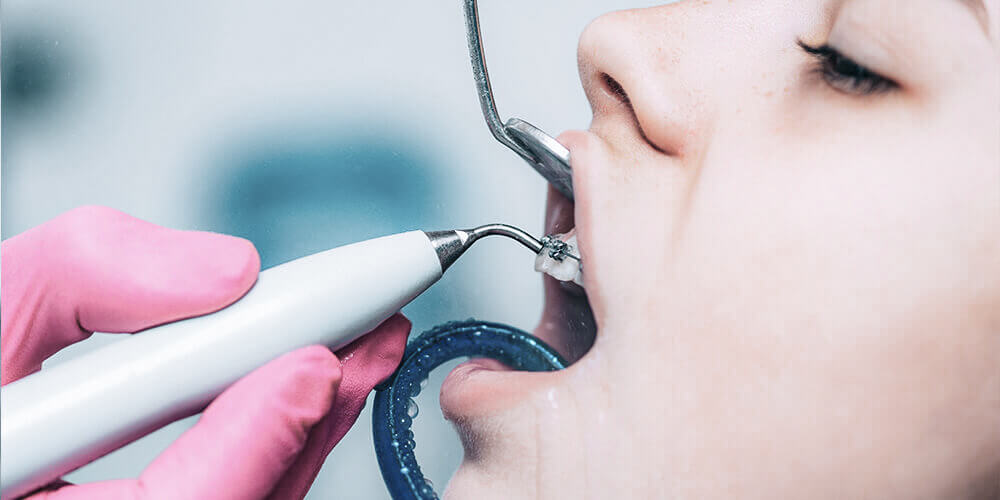
Teeth Cleaning
Routine dental cleanings are an essential part of keeping teeth and gums healthy. Bacteria and plaque can build up on your teeth over time, leading...

Dental Veneers
Veneers are thin, custom-made porcelan shellsdesigned to cover the front surface of teeth to improve your appearance. This is the quick and c...
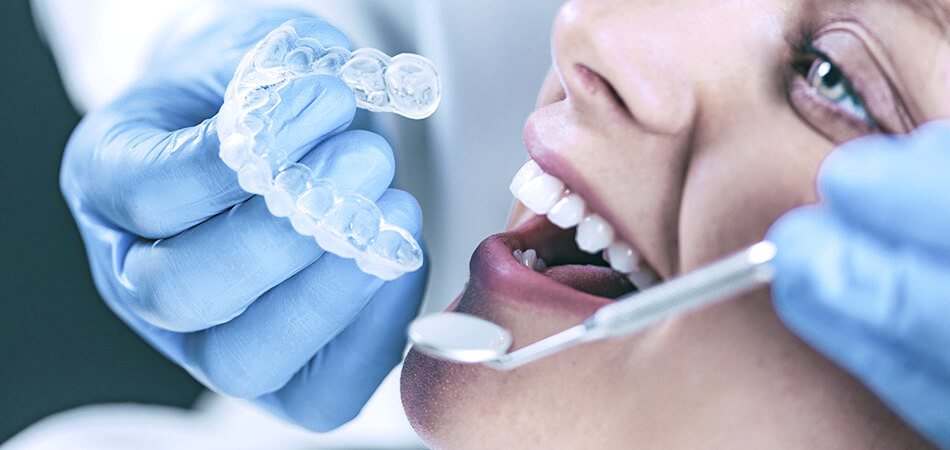
Teeth Whitening
Give yourself a brighter smile! Teeth change color over time. It mostly has to do with our daily routines and habits. Red wine, tea, coffee, ...
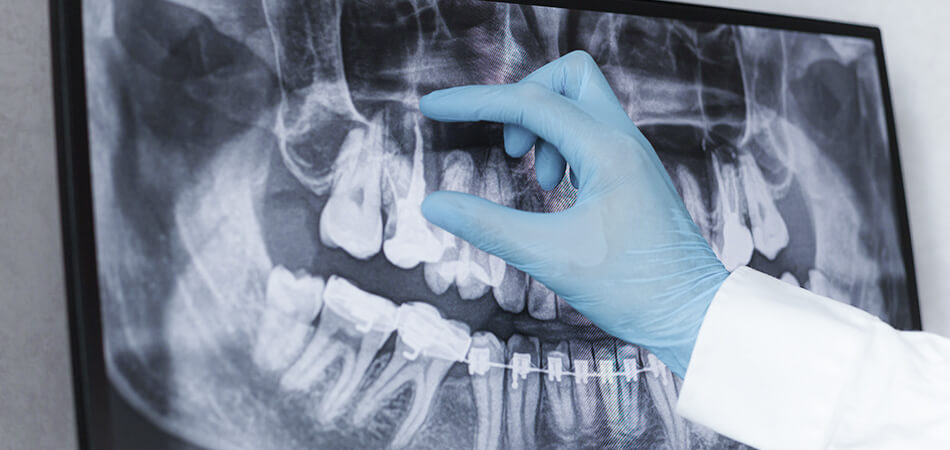
Root Canal
Root canal therapy is a treatment used to repair and save a tooth that is badly decayed or infected instead of removing it. Root canal therap...
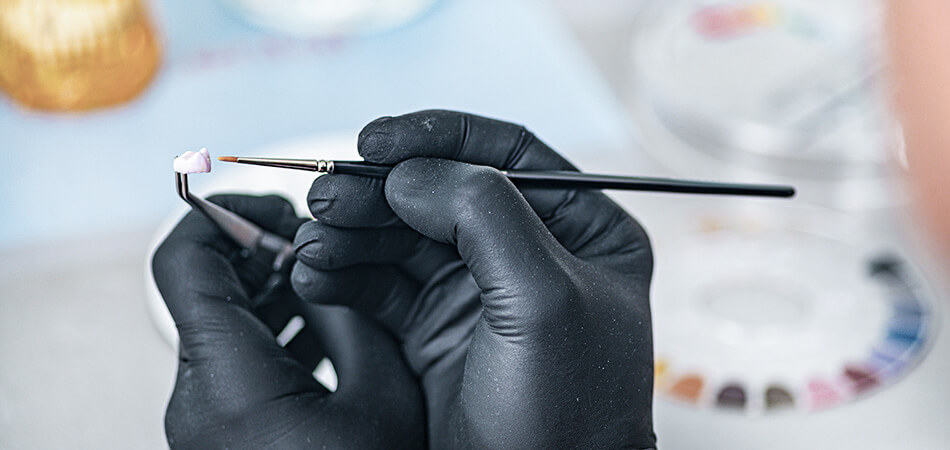
Dental Crowns
Dental crown is a custom-made, permanent restoration that looks like atooth shaped . It is placed over a prepared natural toothto restore its shape, s...
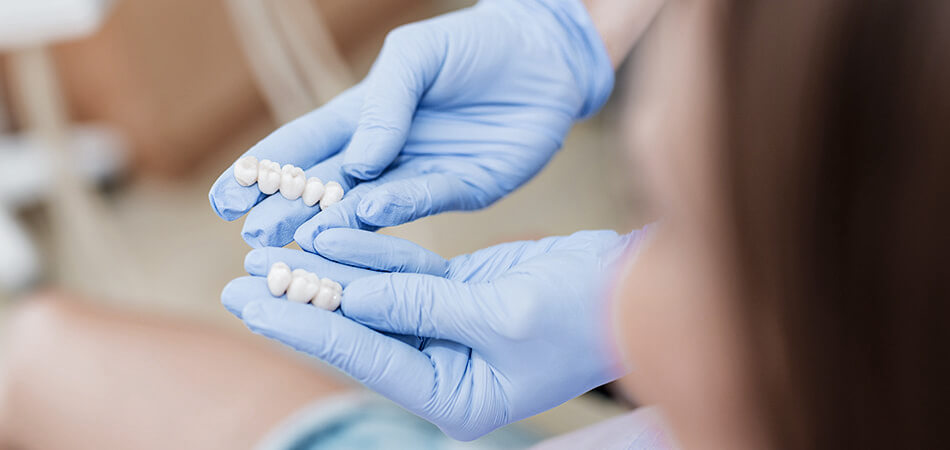
Dental Bridges
A dental bridge is fixed tooth restorationthat is held in place by the abutment teeth oneither side of the gap. Do I need a dental bridge? ...
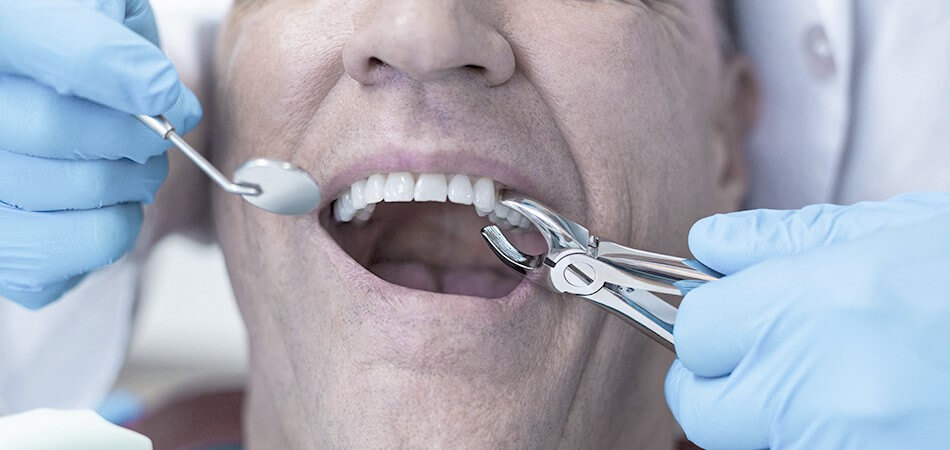
Tooth Extraction
In case of an infection or absces you may need tooth extraction. Pain and swelling are usually signs of an infection or abscess. If the co...
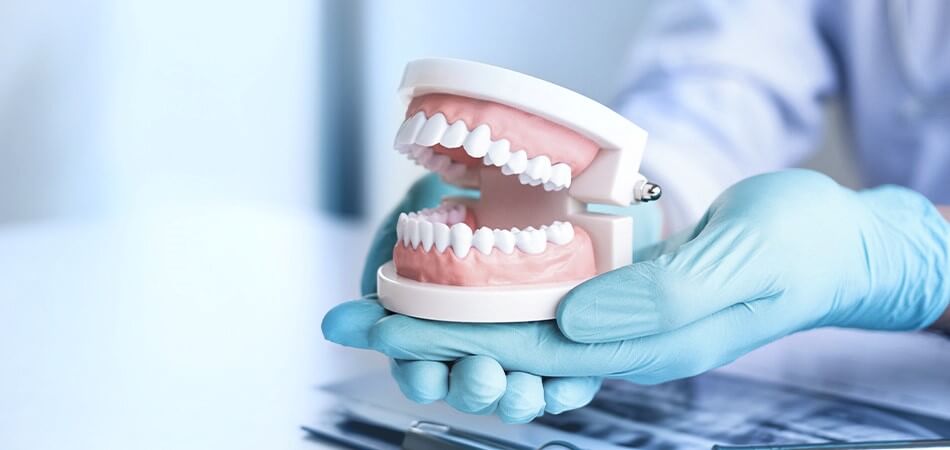
Dentures
Dentures make it easier to eat and speak better than you could without teeth. Dentures are removable appliances that can replace missing teet...